Did you know the lining thickness of a woman’s uterus is crucial for a successful IVF?

Also known as the endometrium, this is where the embryo implants at the beginning of the pregnancy and continues to develop. Every month, when the ovaries release an egg, the uterine lining thickens in size in preparation for embryo implantation. If egg fertilization does not happen, then the lining sheds itself and gets expelled by the body in the form of menstrual blood.

If you are undergoing IVF treatment, your fertility doctor will usually measure the thickness of the uterine lining to ensure that it is adequately thick enough for implantation to occur. This is because the uterine lining is rich in nutrients and provides steady sustenance for the embryo to grow healthily. The ideal thickness of the lining is at least 7mm to 8mm with a trilaminar (three layered) appearance on an ultrasound. A uterine lining that is too thin is not the ideal environment for the embryo, as the embryo may fail to attach properly to the lining and lead to early pregnancy loss.

A woman may have a thin uterine lining for several reasons, the main reason being a deficiency in estrogen, poor blood circulation in the uterus, uterine fibroid, chronic endometriosis (inflammation of uterine lining), hydrosalpinx (blockage of a woman’s fallopian tube), and scar tissues in the uterus.
A thin uterine lining needs to be fixed before a couple tries to conceive. A thick uterine lining is important to sustain a growing fetus. Although it is possible to conceive with a thin lining, your fertility doctor may suggest improving and thicken your lining before the embryo transfer happens.
In many cases, most women are unaware that their uterine lining is thin, as this issue may have been going on for a long time before a woman decides to get pregnant. Proper testing is required to determine this, however, some noticeable signs of a thin uterine lining may be abnormal and painful periods, as well as problems with carrying a baby to full term.
A Thin Uterine Lining can be Fixed by Several Methods

These are tried and tested routines that encourage the growth of your uterine lining to improve your chances of having a successful IVF treatment.
Estrogen Supplements

Estrogen plays an important role in reproduction, and low estrogen levels can sometimes lead to a thin endometrial lining. Estrogen supplements introduce extra estrogen into the body from outside and promotes endometrial lining growth. These supplements can come in the form of patches, oral pills or suppositories.
Physical Exercise

A good supply of continuous blood flow is necessary for the healthy growth of the uterine lining. If you are not previously active, you should engage in regular exercise to improve blood flow. Low to moderate-intensity exercise will do, as high-intensity exercises are not recommended for women who are trying to conceive.
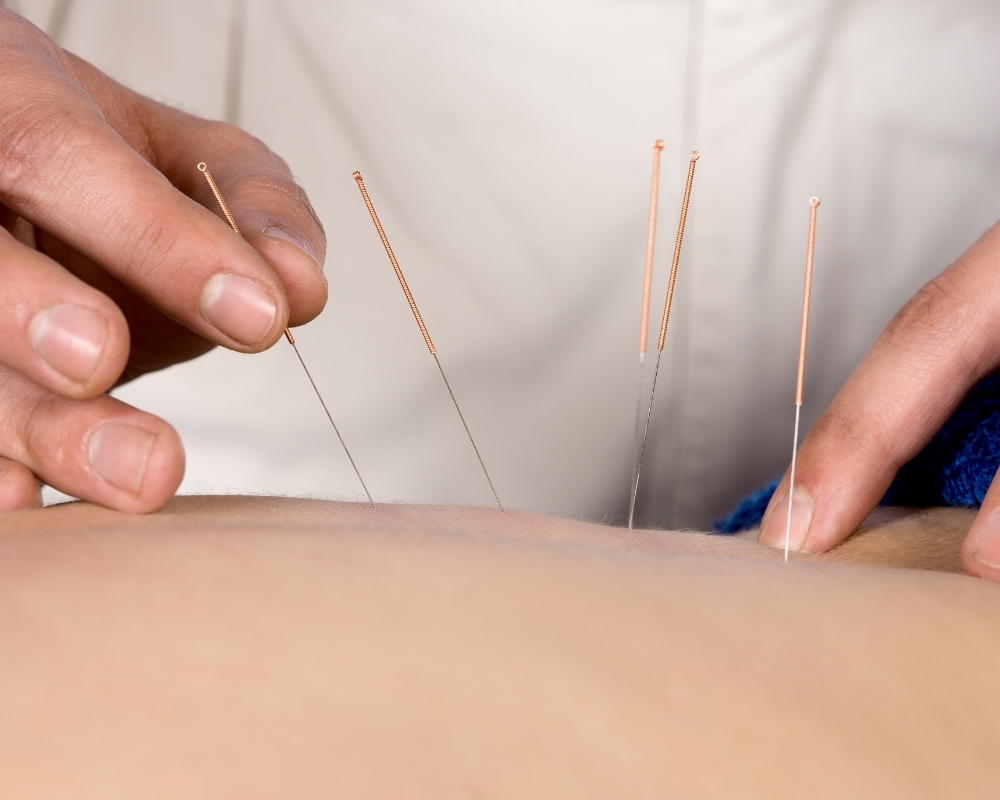
Acupuncture
Acupuncture has been shown to improve fertility in both men and women in several medical studies. Acupuncture increases blood flow to the uterus, improves ovary function, and balances the hormones in the body. This is the key reason why acupuncture has been included in many modern-day fertility treatments.
Quit Smoking and Drinking Coffee

Caffeine and nicotine can impede blood flow in the body and affect blood circulation. If you are able, quit smoking and caffeine entirely. If that’s too challenging, try to cut back on your consumption.
Maintain A Healthy BMI

Women with a low BMI may find it more difficult to conceive because fat cells are responsible for producing extra estrogen in the body. Consider working with a nutritionist to reach your ideal BMI weight, which is usually in the range of 18.5 to 24.9.

As a final word, even if your uterine lining isn’t growing to the ideal thickness, there is still a chance for you to conceive. Be rest assured that as much as you try to plan ahead, some things may not go according to plan. But not all hope is lost. There are plenty of fertility treatments available in the market today, and you should speak to your fertility doctors for more advice.





























 According to Traditional Chinese Medicine beliefs, the best age to conceive is 25 to 29 years old for women, and 27 to 35 years old for men. At this age, men and women are generally more stable physically and emotionally, not to mention financially! Research has shown that early and late pregnancies (earlier than 20 or after 35) tend to have a higher mortality rate and increased risk of birth defects.
According to Traditional Chinese Medicine beliefs, the best age to conceive is 25 to 29 years old for women, and 27 to 35 years old for men. At this age, men and women are generally more stable physically and emotionally, not to mention financially! Research has shown that early and late pregnancies (earlier than 20 or after 35) tend to have a higher mortality rate and increased risk of birth defects. Research shows keeping a healthy weight plays a huge role in fertility, as being overweight or obese actually decreases fertility in men and women alike.
Research shows keeping a healthy weight plays a huge role in fertility, as being overweight or obese actually decreases fertility in men and women alike. Female fertility is complex and could stem from various reasons, but male fertility is surprisingly easy to resolve by leading a healthy lifestyle. Did you know smoking causes a decline in sperm count, reduces sperm motility (the sperm’s ability to swim), and abnormal sperm shape as well? When a man quits smoking, he will be able to see improvement in his sperm count in just 3 months.
Female fertility is complex and could stem from various reasons, but male fertility is surprisingly easy to resolve by leading a healthy lifestyle. Did you know smoking causes a decline in sperm count, reduces sperm motility (the sperm’s ability to swim), and abnormal sperm shape as well? When a man quits smoking, he will be able to see improvement in his sperm count in just 3 months. Sperm is damaged by high temperatures, and this is one of the reasons why the male reproductive organs are outside of the body – the scrotums need to be kept cool and lower than our normal body temperatures (36.5 °C)
Sperm is damaged by high temperatures, and this is one of the reasons why the male reproductive organs are outside of the body – the scrotums need to be kept cool and lower than our normal body temperatures (36.5 °C)